Cutting Edge Technology
At Hawkesbury Optometric, we pride ourselves on providing all of our patients with the highest standard of care. To help us do this, we use revolutionary technology to detect and diagnose vision problems, diseases, and other serious conditions early, so that steps can be taken to prevent or limit vision loss.
When was your last eye exam?
Retinal Imaging
Retinal imaging allows your optometrist to take a detailed picture of your retina, often alleviating the need for dilating drops. Retinal imaging allows your optometrist to detect and track subtle changes in your eyes that may indicate something is wrong.
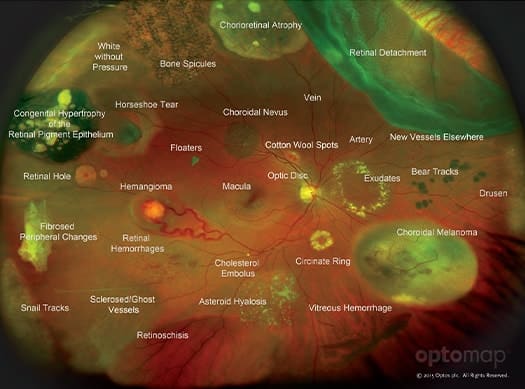
At Hawkesbury Optometric, we use an Optomap ultra-widefield retinal camera. This amazing piece of technology allows us to view your entire retina to ensure it is healthy. Early detection is critical, as many retinal conditions and other forms of eye disease can be slowed or stopped with early detection.
Our Optomap includes Fundus Autofluorescence (FAF), a revolutionary imaging technique that uses the natural fluorescence of the retinal pigment epithelium (RPE) to create an even more detailed and accurate picture of your retina. FAF is used to pinpoint dying or dead tissue, which can give your optometrist greater insight, even sooner than a colour fundus image alone.
FAF is particularly useful for diagnosing age-related macular degeneration.

Optical Coherence Tomography (OCT)
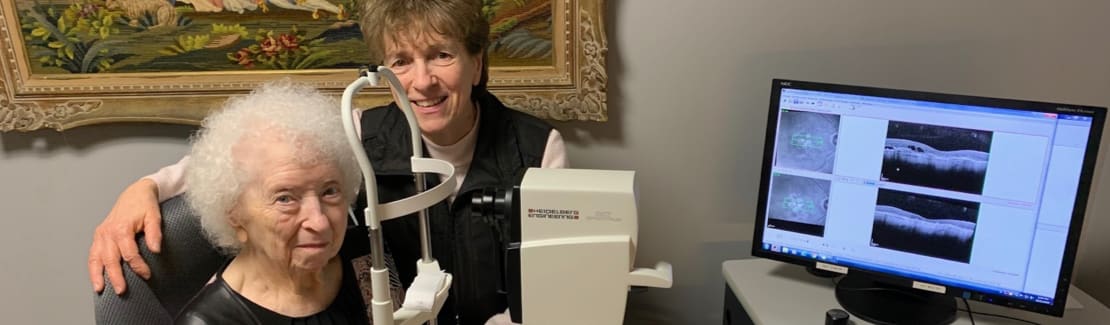
Optical Coherence Tomography is an advanced technology that can benefit patients of all ages. OCT uses light to give your optometrist a cross-sectional view of the different layers that make up the retina at the back of your eye.
Since purchasing our Heidelberg OCT in 2012, we have been able to provide more detailed scans of our patients’ eyes. Never before has one instrument been able to capture so much detail with an accuracy of 1/1000 of a millimetre. This accuracy makes it easier than ever to diagnose serious eye conditions such as glaucoma, age-related macular degeneration, and retinal disorders, as well as detect systemic conditions, such as diabetes.
In 2015 we upgraded our OCT with the latest Spectralis software, adding a whole new dimension of accuracy to our glaucoma detection process. This revolutionary software uses state-of-the-art algorithms and unique scan patterns to more accurately detect signs of glaucoma. As with any eye disease, early detection is critical to preserving vision.
This advanced piece of equipment allows us to electronically send information through the Care1 Electronic System to specialists like the Ottawa Retina Center allowing them to confirm our diagnosis and arrange follow up visits more quickly, facilitating urgent retinal care and offering our patients peace of mind.
Non-Contact Tonometry (NCT)
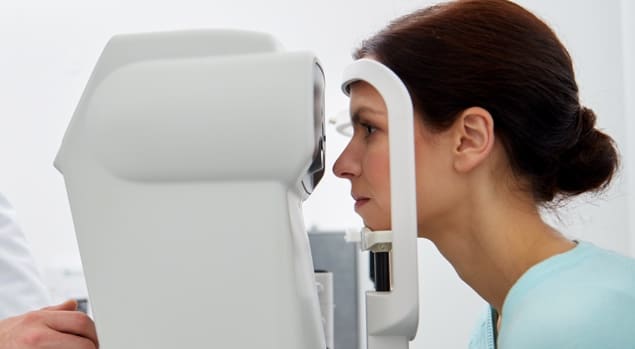
Non-Contact Tonometry, more commonly known as the “air puff test”, is used to measure your eyes internal pressure (called your intraocular pressure or IOP). It measures your eye’s resistance which if high, may be a sign of elevated intraocular pressure. Your optometrist uses this information, in addition to other tests and procedures, to determine your risk of developing glaucoma.
Pachymetry

Pachymetry is a quick test that uses ultrasound to measure your corneal thickness, which can affect the accuracy of tests such as non-contact tonometry (NCT). Thicker corneas offer more resistance, which means that the NCT may incorrectly flag you as having a high intraocular pressure. If your optometrist knows you have thick corneas, they can calibrate the test accordingly, producing more accurate results.
On the other hand, if you have thin corneas, you have an increased risk of developing glaucoma. According to the Ocular Hypertension Treatment Study, Pachymetry is the single greatest predictor of glaucoma. Patients with thin corneas and a family history of glaucoma can be scheduled for further testing as a precautionary measure.
Pachymetry is also useful for determining if your corneas are sufficiently thick to undergo laser eye surgery.
Visual Field

Visual field testing is used to measure your peripheral vision. There are a variety of conditions and diseases that can impact your peripheral vision, including glaucoma, diabetes, and optic nerve disease. It is also used to detect diseases that affect the visual pathway from your eyes to your brain and vision loss due to injury.
This vital test only takes about three minutes, but it is critical for safeguarding your vision. According to the Ocular Hypertensive Study, almost a third of patients that developed glaucoma, showed a field defect as their first sign of disease.
Slit Lamp

This technology has greatly evolved. Now with photo documentation, special filters and IR light built into the device, many different conditions affecting vision can be diagnosed, including dry eye, inflammation, and cataracts.
VX-40

Using this technology on all our patients, we can demonstrate a good quality vs a poor quality progressive lens! Not all progressives are made equal and this tool helps solve many adaptation problems. This is a great coaching tool, and sets reasonable goals for achieving successful patient satisfaction!
Autorefractor
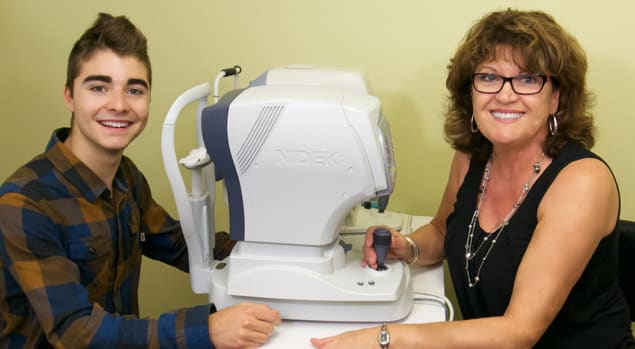
The autorefractor is used to automatically estimate your prescription. Like a manual refractor, the autorefractor works to determine the lens power required to accurately focus light on your retina, providing you with clear vision. The autorefractor is particularly useful for determining the prescription of young children and other patients who may have difficulty sitting still, paying close attention, or providing the feedback your optometrist requires to perform a manual refraction accurately.